***
"Red State Moocher Links"
***
Published: Friday, 2 Aug 2013 |
By: Dan Mangan | Health Care Reporter

Jon Schulte | E+ | Getty Images
Some states may be "blue" in more ways than one after Obamacare really kicks in next year.
A major deal on the Affordable Care Act could lead to an ironic outcome: more residents in red states than in blue enrolling in Obamacare health insurance exchanges.
That's because the federal government, which is running health exchanges in nearly all the red states, is moving to allow several for-profit online insurance markets to sign up subsidy-eligible people in the exchanges' insurance plans.
(Read more: Landmark Obamacare deal)
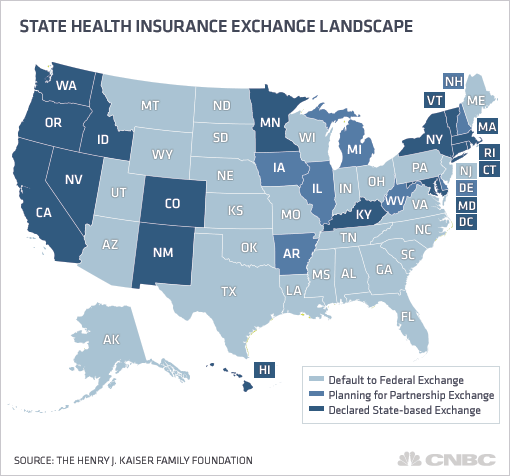
But a CNBC.com survey shows that nearly all the 14 states (and District of Columbia) running their own exchanges have rejected partnering with for-profit Web markets to augment their enrollments. Those states, which mostly voted for President Barack Obama, represent about 40 percent of U.S. population, and include New York and California.
"I think Web brokers will assist in facilitating enrollment, hands down, so states who do not partner with Web brokers will, I think, have less enrollment," said Christopher Condeluci, an employee benefits lawyer with the firm of Venable.
Condeluci said he estimates states that run their own insurance exchanges without Web partners could have up to 25 percent fewer people signing up than the federal-run exchanges. Enrollment begins Oct. 1., and coverage starts Jan. 1.
Lower enrollment means "you don't have enough people in the risk pool," which would drive up premiums in future years, Condeluci pointed out. "Rates are just going to be higher."
Obamacare raising costs for cancer care?
The Congressional Budget Office says delaying the Obamacare employer mandate will cost taxpayers an extra $12 billion. And Dr. Scott Gottlieb, an American Enterprise Institute fellow, says Obamacare could jack up the cost of cancer treatment. With with CNBC's Josh Lipton.
Many of the blue states running their own exchange gave a range of explanations for refusing to partner with eHealth, GetInsured.comand other Web markets. They included difficulties in setting up technical links with the markets, concerns about privacy protections and worries that the markets would rush customers through the enrollment process.
John Kelly, principal business advisor at health-care IT solutions provider Edifecs, said that the "core technology is fairly straightforward" to create online links between state exchanges and private Web markets.
If partnering with the online markets is a priority for state exchanges, "they could make it happen sooner than later," he said, adding that it's reasonable, however, for states to defer as they scramble to get their own exchanges ready to open Oct. 1.
Protecting data
"We sat down and looked at this long and hard," said T.J. Bowden, spokesman for Nevada's health exchange, which decided to forgo a deal with Web markets because of concerns about the security of enrollees' information as it was transferred between the markets and the exchange.
(Read more: Obamacare: A new opportunity for fraud?)
"If we have a loss of data with one person, we lose trust of the consumers," he said.
Connecticut's exchange, Access Health Connecticut, likewise rejected such deals. "We're trying to keep as much control as we can" over the enrollment process, said CEO Kevin Counihan. "We just want to make sure that we can control ... access to information and that we hand-hold people through what is a very complicated process."
Despite widespread opposition by state-run exchanges to using Web markets to supplement enrollment, both eHealth's Lauer and GetInsured.com CEO Chini Krishnan told CNBC they will continue lobbying those states.
"By engaging with Web-based marketplaces like Getinsured.com, states can leverage the relationships we are building with retailers and other brick-and-mortar chains to service both on- and off-exchange customers," Krishnan said. "Ultimately, this brings them scale and operational leverage."
Lauer dismissed the technical excuses offered by the states. "A college freshman taking an introduction to computer science course could make the technology connection in each state for us to enroll people online," he said.
He also rejected the arguments about security concerns—which the federal government has said were satisfied in the deals they made this week—and has repeatedly cited eHealth's long track record in enrolling individuals in insurance plans as proof that the company is well-suited to partner with the government-run exchanges.
"I'm not going to relent," Lauer said. "I'm not going to stop unless we get all these states there, because I think this is the way to go."
—By CNBC's Dan Mangan. Follow him on Twitter @_DanMangan.

No comments:
Post a Comment